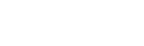
Each year in the United States, approximately 50 to 60 children are born with 5p- Syndrome (five p minus), also known as Cat Cry Syndrome or Cri du Chat Syndrome. 5p- Syndrome is characterized at birth by a high pitched cry, low birth weight, poor muscle tone, microcephaly, and potential medical complications. “5p-” is a term used by geneticists to describe a portion of chromosome number five that is missing in these individuals. 5p deletion is a spectrum disorder.
Children born with this rare genetic defect will most likely require ongoing support from a team of parents, therapists, and medical and educational professionals to help the child achieve his or her maximum potential.
Years ago, it was common to place children with 5p- Syndrome in institutions with other severely developmentally delayed individuals. During the early 1980s, research revealed that those raised in family settings with the benefit of early intervention programs made remarkable progress, far exceeding the expectations of doctors who first described the syndrome.
Most individuals who have 5p- Syndrome have difficulty with language. Some become able to use short sentences, while others express themselves with a few basic words, gestures, or sign language.
Nearly all children with 5p- Syndrome have poor muscle tone when they are young. Other characteristics may include feeding difficulties, delays in walking, hyperactivity, scoliosis, and significant cognitive delays. A small number of children are born with serious organ defects and other life threatening medical conditions, although most individuals with 5p- can anticipate a normal life expectancy.
Both children and adults with this syndrome are usually friendly and happy, and enjoy social interaction. With early and consistent educational intervention, as well as physical and language therapy, children with 5p- Syndrome are capable of reaching their fullest potential and can lead full and meaningful lives.
For additional information, please contact us here.
New Families
Don’t panic!! It’s okay to cry; it’s okay to grieve; it’s okay to vent.
After the diagnosis the parent will most likely see a genetic counselor. Depending on the counselor’s experience, he/she may or may not give accurate information. 5p- deletion is a spectrum disorder. Individuals with this syndrome will range from mild to severe in developmental delays. Symptoms may not be present in all individuals. The location and type of deletion (“de novo,” mosaic, unbalanced translocation), early intervention and various therapies, and the natural variation among people all play a key role in your loved ones development. Individuals with this syndrome will have his or her own timeline meeting developmental milestones. It will be hard not to compare the child with Cri du Chat Syndrome with other “normal” children his or her age. Children with Cri du Chat Syndrome have a higher receptive than expressive language. They may surprise you and do a lot more than what you will be told.
Before too long parents become the experts on the syndrome. They will know more about the syndrome than the doctors, the therapists, or the teachers. They become the great educators!! Parents will soon learn terms they didn’t even know existed, and will become advocates and the voice for their child.

Parents should look into early intervention, speech therapy, physical therapy, and occupational therapy. Sign language and other forms of communication through devices should be introduced early in the child’s life. A child with Cri du Chat Syndrome will learn and retain more than what they are able to express. Because of this a child will become frustrated and may develop undesirable behavioral issues. Parents, therapists, and educators should all work together in the overall education of the child and create sustainable goals. The accomplishment of simple goals and milestones are to be celebrated!! Focus more on what the child can do and not so much on what one is told they cannot or will not do!
It is crucial for parents to network successfully through the global Cri du Chat Syndrome support organizations to gain a sense of relief, and to realize that they are not alone in their journey. By developing links with other families of individuals with the syndrome, parents learn that a wide variation exists in ability levels for individuals with Cri du chat Syndrome at all ages. Families are able to access strategies that have worked with other children with the syndrome. Parents are encouraged to use a total communication approach and to encourage their children, who typically tend to be complacent, to work. Knowing about different abilities between children may encourage families to participate in intensive early educational training.
Characteristics
What are the characteristics of Cri du Chat Syndrome?
- A cry that is high-pitched and cat-like
- Low birth weight and slow growth – failure to thrive
- Small head circumference (microcephaly)
- Small jaw (micrognathia)
- Wide-set eyes
- Downward slant of the eyes
- Extra fold of skin over the inner corner of the eye (Epicanthal Folds)
- Low-set or abnormally shaped ears
- Skin tags
- Partial webbing or fusing of fingers or toes
- Single line in the palm of the hand (simian crease)
- Low muscle tone
Other characteristics and symptoms include:
- Cognitive delays
- Gross motor delays
- Fine motor delays
- Speech and language delays
- Inguinal hernia
- Constipation
- Sleeplessness
Diagnosis
How is Cri du Chat Syndrome diagnosed?
Cri du Chat syndrome is diagnosed by a blood test that is put through a full genetic testing.
There are various tests that can be used to determine if your child has Cri du Chat Syndrome. The first is a simple Chromosome Analysis also known as a Karyotype. The Karyotype will map our your chromosomes and will let you know if something is missing (or added). An example of a karyotype for Cri du Chat Syndrome would be: 46,xx,del5p14.2. To translate this it would be as follows: the number “46” means that you have 46 chromosomes (23 pair); “xx” in this case means it is a girl with two “x” chromosomes (a boy would be “xy”); del5p indicates that there is a deletion on the 5th chromosome, “p” arm. A chromosome consists of a “p” or short arm and a “q” or long arm and then the centromere which is in the area where the “p” and “q” connect. Next the 14.2 is the location on the “p” arm that the deletion has occurred.
Another test that is being used is called FISH testing. FISH stands for fluorescence in situ hybridisation. This test looks for gene changes in cells. Genes make up your DNA and control everything the cell does, including when it grows and reproduces. FISH tests look for specific genes or parts of genes. The FISH test can also be used when providing a diagnosis for Cri du Chat Syndrome and may provide a very similar karyotype as above.

A third test, and also the newest testing that families are seeing done with their children, is called Chromosome Microarray Analysis. A Microarray analysis is a DNA-based method of genetic analysis, used to identify significant chromosome abnormalities. The way it works is a DNA sample is prepared and hybridized to a glass slide. Then a large number of molecular probes are arrayed. The probes have small segments of DNA from the patient and are compared to a control DNA. This type of analysis is able to diagnose deletions and duplications of whole chromosomes, portions of chromosomes, and specific locations. A chromosome analysis from a Microarray will have more information on it and will provide you with the exact location of the deletion or duplication.
Development
Here’s some things to look for when it comes to development with 5P- syndrome.

- Gross and fine motor skills
- Expressive speech and language delays
- Communicate by sign language, communication devices, gestures and a few basic words
- Poor muscle tone (hypotonia)
- Slow growth associated with failure to thrive
- Constipation
- Low Birth weight
- Normal Life expectancy
- Young adults may have premature graying
- Most children walk, although at a slower pace and with a guarded gait.
- Majority of children do not achieve toilet training.
- Many children and adults have sleep issues.
- Some have visual problems.
- 80% of children have a hearing condition known as hyperacusis (hypersensitivity to noise).
- Children with CdCS undergo typical changes in puberty at the appropriate age
- Many children have seizures ranging from Grand Mal to silent.
- Very few adults are able to work with supervision.
- Even fewer adults are able to live independently.
- Most children with CdCS have behavioral issues
- Attention Deficit Hyperactivity Disorder (ADHD).
- Poor concentration.
- Impulsiveness and OCD.
- Biting, hair pulling, pinching and hitting.
- Temper tantrums, stubbornness, frustration, self-biting, head banging and skin picking.
- Autistic-like characteristics- some are dually diagnosed with Autisim.
- Hand flapping, string twirling and rocking.
Additionally, you can find out more by looking at the following:
Treatment
Occupational therapy
Occupational therapy benefits our kiddos by providing fine motor, visual perceptual, self-care and sensory integration intervention to assist the child/young adult to maximize their skills, develop new skills and be able to relate more effectively to the environment around them. Occupational therapists who work with children have education and training in child development, neurology, medical conditions, psychosocial development, and therapeutic techniques.
Physical Therapy
Children with Cri du Chat syndrome may experience physical difficulties during their growth and development. Physical therapy can help your child’s physical development in the following ways: helping them to sit, stand, improve fine motor skills, etc. The goal of physical therapy for children is not to speed up the rate of their development, but to facilitate the development of optimal physical movement.
Speech Therapy
Speech therapists work with children from an early age to aid in swallowing by providing advice on what best methods exist for feeding. As children with Cri du Chat syndrome grow older, they may experience problems with their speech. Speech therapists provide guidance on assisting children with communication issues by utilizing and teaching different methods of communication such as: sign language, picture exchange system, technology assisted communication, etc.
Alternative Therapies
Many families have found the use of alternative therapies as a way to complement Occupational, Physical and Speech therapy. Here is a list of therapies that other children and/or adults with the syndrome have benefited from:
- ABA Therapy (Applied Behavior Analysis)
- Adaptive Physical Education
- Aromatherapy
- Aquatic Therapy
- Behavior Therapy
- Cranial Sacral Therapy
- Dolphin Therapy
- Hippo-therapy (also known as Horse Therapy)
- Music Therapy
- Play Therapy
- Pragmatic Group Therapy
- Sensory Learning Therapy
Frequently Asked Questions
Click on the + to see responses.
What things did you do to help toilet train your child?
It’s hard to know when your child will be ready to be toilet trained. One thing to remember is that being able to use the toilet requires the child to not only be cognitively ready but also physically ready. Because our children are known to have low muscle tone a child may not be able to physically be able to use the toilet until a bit older. So when do you know when to start? Here are some ideas from parents like you:
- Wait until they can sit unassisted;
- Take them with you when you go to the bathroom and talk to them about what you are doing;
- Take them to the bathroom every 30 minutes – schedule training. Can be used at home and at school;
- Chapter on Potty Training in a book called “Steps for Independence”
- Patience and persistence. Many children are not potty trained until they are ready (average age 9 years old)
- Constant reminders
- Teach them the sign for potty and reward them when they use it successfully (sticker chart)
- Ask the 5p- Society for the handout given at the 2012 Denver conference on Potty Training
- Purchase a removable potty seat – ideas include
- www.onestepahead.com/wooden-family-toilet-seat.pro
- www.pottytrainingconcepts.com
- Mayfair 83EC 000 NextStep Child/Adult Built in Potty Seat (sold on Smile.Amazon.com)
My child is constipated, what can I do to handle chronic constipation?
One of our parents, Tammy Dawson, wants to share her experience with PROBIOTICS.
“Many of our sons and daughters battle with constipation issues. My son, Allan, has fought this issue all of his life. We have tried mineral oil, prune juice, enemas, daily doses of Miralax, and adding extra fiber as much as possible with no luck. The norm for him has been having perhaps one bowel movement every seven days which we all know would be discomforting to say the least. I have been looking for answers to help him find relief in this area.
“I honestly believe that our sons and daughters just learn to live with this chronic condition, as uncomfortable as it must be. I have even thought to myself that it may play a role in their behavior issues, which so many seem to have at a younger age, at least for my son it was far more difficult. Like so many of you, we have had this discussion with our doctors over the years about how to overcome the constipation issue and all I ever got from our primary doctors as well as specialists was to add more fiber and take Miralax daily which, as we all know, if taken daily will only lead to loose runny stools and a mess and headache for those who are caring for them. So while using that method I had to try and find the right dosage to give Allan. And here again this would basically only lead to one bowel movement on a weekly basis. I also started giving him active yogurt and more peaches and pears as a part of his daily diet.
“Then recently I discussed with my gastro specialist this matter not only about myself as a IBS sufferer but about constipation in general. I was told to research “Probiotics” and that they are finding this dietary supplement to be a relief to many who suffer various digestive issues that often lead to constipation or diarrhea.
“So I took his advice and did some research and spoke with a friend of mine who is into all natural holistic medicine/treatment. She said it saved her from having to take various prescription medications for her issues and has given her much relief over the last couple of years. So long story short, I took Allan to see his primary doctor because I have been finding him sitting on the toilet for hours at a time struggling to have a bowel movement and she also informed me that I need to start him on probiotics. She said we should see a change very soon. So Allan and I left there and went to a local drug store and I ended up purchasing Nature’s Bounty Ultra Strength Probiotics and gave him the recommended dosage in the car and went about our business. We were out running errands and Allan informed me he had to go “pooh pooh” so we went home and sure enough he had a bowel movement. At that time I gave no thought to it. I was just thinking it was time.
“I give the probiotic to Allan each day when he arrives home from school, and sure enough he has a bowel movement every night. So a week went by and I was thinking perhaps this is a coincidence. The second week went by and he was still continuing to go each and every day. This now has been going on for approximately 6 to 8 weeks. I have been very happy with the results. For us it has been a life saver. I will say though that I thought I would buy in bulk at Costco a different brand. But that brand did not work for Allan. I had a difficult time finding the original product so I ordered online. Sure enough as soon as it arrived, I gave Allan the recommended dosage and he had a bowel movement within 3 hours. If you decide to give this a try you may have to find a brand that works for you.
“I have heard that for some people refrigerated probiotics are supposedly even better but I figured if it isn’t broke why fix it for now. So my advice would be, if you are looking to administer to anyone younger than 18, discuss with your Pediatrician or doctor before giving to your child. I hope that I have shed some light in regards to possibly finding something that will actually conquer our sons/daughters constipation issues. And perhaps in due time we will find out if indeed this is something that definitely needs to be a part of our children’s daily diets. Good luck to you all.”
Will my child ever speak? What techniques did you use to facilitate verbal speech?
There is no guarantee that your child will develop verbal speech. It is recommended that you begin sign language with your child as soon as possible. Learning how to communicate at a young age will assist in language development. If a child is able to speak verbally they may not have intelligible speech and known the sign can help with being understood. Some children who do have verbal speech are only intelligible to their parents and those close to them. Ideas to help facilitate verbal speech include:
- Flashcards
- Reading to the child out loud
- Reading/language apps
- Speech/language therapy as soon as possible
One parent used a magna doodle (magnetic board) and would write a word or letter, say the word or letter, sign the word or letter and then erase the word or letter and repeat it until the child understood it or was able to say it (this child did develop intelligible speech).
Children with Cri du Chat Syndrome have aggressive and/or self- injuring behaviors. They are known to hit, kick, bite, pull hair of others, but also to pick at their skin, head bang, pull out their own hair, etc. What has worked for you to help with these behaviors?
Most children with the syndrome will exhibit some of these behaviors. Many will exhibit all of these behaviors. It is very difficult to know what to do when a child exhibits these behaviors. Trying to figure out the root of the problem that is causing the behavior can be exhausting. Some parents provide the child with a redirection such as soft hands or jumping (see more on self-injurious behaviors below).
Most of the behaviors are communication based. The child has the inability to communicate his or her needs and gets frustrated. It is recommended to begin to facilitate communication with your child when still an infant. Start with sign language and teach them basic communication signs such as “more”, “drink”, “eat”, “play”, etc. Children with Cri du Chat Syndrome also need a lot of vestibular movement and could be one of the reasons that they head bang. Try swinging the child when they are feeling tired and overstimulated.
AmySue Reilly, a member of the Professional Advisory Board and conference presenter on Effective Positive Behavior Modification asks ‘What can one do to change a child’s behavior? She tells us that children tend to 1) continue a behavior when it is rewarded and stop a behavior when it is ignored. She also tells us that 2) consistency in your reaction to a behavior is important because rewarding and punishing same behavior atdifferent times confuses your child. Some of her recommendations are:
- Make a short list of important rules.
- Avoid power struggles, no-win situations and extremes.
- When you think you’ve overreacted, it’s better to use common sense to solve the problem.
- Even if you have to be inconsistent with your reward or punishment method, avoid doing this often as it may confuse your child.
- Accept your child’s basic personality, whether it is shy, social, talkative or active.
- Basic personality can be changed a little, but not very much.
- Try to avoid situations that can make your child cranky, such as becoming overly stimulated, tired or bored.
- Don’t criticize your child in front of other people.
- Describe your child’s behavior as bad, but don’t label your child as bad.
- Praise your child often when he or she deserves it.
- Touch him or her affectionately and often. Children want and need attention from their parents.
- Develop little routines and rituals, especially at bedtimes and meal times. Provide transition remarks (such as “In 5 minutes, we will be eating dinner.”) Allow your child choices whenever possible. For example: “Do you want to wear your red pajamas or your blue pajamas to bed tonight.”
What do you do about constant picking and chewing?
We all know our children do not fit in a “one answer fits all” box but here are some suggestions that have worked for many families. First, you have to figure out, as with all behavior, why are they doing it or what are they getting out of it? If the answer is just a “nervous habit” or sensory issue, there are a few things you can try. First try finding something you can replace their self-injurious behavior with, such as for biting, there is Chewerly they can use. The key to self-injurious or inappropriate behavior is not always getting rid of it but finding a harmless, appropriate replacement behavior to relieve that need. Many of our children will use their shirts to bite, which leaves huge holes. For biting, if your child is able, provide them with “hard munchable” snacks to help stimulate the nerve in the jaw, where they are seeking input. Some examples of hard munchables are raw carrots or Snyder hard pretzels. Snyder pretzels also sell hard pretzel flavored bits. The flavor can help with an additional sensory input of strong flavor, if your child likes it. TalkTools, Inc. also have chewy tubes in different degrees of toughness, depending on your child’s needs. Have your child’s Occupational Therapist do a Sensory Evaluation on your child to help develop a sensory diet. The OT can also recommend the right equipment and level of equipment that would work best for your child.
Picking can be a bit trickier. In general, it starts with a mosquito bite or sore, which they itch and pick until it becomes a large sore or infected. We have had some great creative ideas parents have used to allow time for the sore to heal. First, make sure your child’s nails are cut short. Next, use medications to help with the itch, either cream, oral, or both. Finally, this is where creativity comes into play. One Parent suggested using liquid Band-aid to help the sore heal and protect it. Another has put multiple Band-aids on their arm/leg and let the child “pick” off the band-aids. Small bubble wrap to pop, Tag blankets (with the small tags along the borders) have also been suggested to help keep their hands busy. Others have put Band-aids, socks or gloves over their child’s fingers/hands to help prevent scratching.
As with any issues your child has, make sure you are working closely with your therapist(s) in your area to develop the most accurate and up to date plans to best help your child.
Will my child ever walk on his/her own?
Most children with Cri du Chat Syndrome will learn to walk. It may take a lot longer than the average child. Many children that do walk tend to walk by the time they are 5 years old. Early intervention and physical therapy is essential. Please keep in mind that children with CdCS have low muscle tone. They most likely won’t be ready until the muscles are strong enough to hold them up. Here are some ideas from some of our parents.
- A harness has been developed by a mom of a disabled child that attaches to the parent’s leg and simulates walking for the child. Check it out here.
- Bumbo seat – this is a great piece of equipment for short periods of time (feeding, fine motor activities) but it places your child in a very large base of support and requires your child to utilize no truck musculature. (Kelly M DiNoia, MPST, Med and Abe Mathews, CPO, 5p- Society conference 2013).
- The Right Height Chair – this is a stylish seating system developed for children and teens with mild to moderate physical involvement. The chair is designed to grow with your child from 6 months up to 250 lbs! The chair offers secure positioning support with a sleek, modern design to create a chair that will fit into any home. It is the perfect seating solution for your child at home, school, therapy or daycare center. (Kelly M DiNoia, MPST, Med and Abe Mathews, CPO, 5p- Society conference 2013).
- Standers – many parents are so excited about having their children stand. The problem is for a child that we believe will be ambulatory the stander gives the child the idea that they need to lock their joints to stand. Later this becomes an issue for low tone children, they later have difficulty standing without their joints locked. It also becomes an issue with ordering dynamic equipment later. (Kelly M DiNoia, MPST, Med and Abe Mathews, CPO, 5p- Society conference 2013).
- Gait Trainer -the Rifton Pacer Gait Trainer or the KidWalk, are uniquely adjustable for different needs and levels of development. Pediatric walkers are used when a child is already able to bear weight-bearing strength, and develop a healthier gait. The Gait Trainer supports prompts enable active participation and promotes valuable motor learning, strength gains and adaptive mobility. As a child or adult gains skills, improves function & achieves greater independence, the supportive prompts of the gait trainer can be easily removed.Gait trainers are customizable and unique. It helps clients improve their walking pace through practice, while helping them develop, heal, and become more independent at their own pace. (Information provided by Kelly M DiNoia, MPST, Med and Abe Mathews, CPO, 5p- Society conference 2013).
- Posterior v. Anterior Walkers – Posterior walkers are widely used in the pediatric population, with literature providing evidence of improved gait efficiency, a more normalize strike length, and more optimal upright posture during ambulation. An anterior walker is often used with individuals with special needs that need to lean forward to propel themselves, but have a difficult time maintaining their balance while doing so. (Kelly M DiNoia, MPST, Med and Abe Mathews, CPO, 5p- Society conference 2013).
- At the 2013 conference in New York, Abe, Mathews, CPO with Progressive O & P, to talk about Orthosis, an external device with controlling forces needed to 1) Improve body alignment, 2) Improve function, 3) Immobilize an area, 4) Protect a joint or limb, 5) Reduce Pain, and to 6) Prevent the progression of a deformity. What type of Orthoses are there? 1) foot orthotic, UCBL, SMO – Supra Malleolar Orthoses, AFO – Ankle foot Orthosis, 5) Hinged AFO and KAFO – Knee Ankle Foot Orthosis.
Help?? My child won’t sleep. What works?
A commonality among most of the children and adults with Cri du Chat syndrome is the lack of sleep!! Here are a few suggestions by parents on our Facebook page:
- White noise (sound machines)
- Essential oils like Lavender
- Melatonin
- Prescribed sleep aides
- Strict sleep schedule
What type of feeding difficulties do children with Cri du Chat Syndrome have?
There could be a number of feeding difficulties that a child with the Syndrome can have. Because children with the syndrome have low muscle tone there could be difficulty with sucking and using the correct muscles. However, more severe issues are reflux and aspiration. Many children with the syndrome have had swallow studies and the insertion of feeding tubes. If you child does have a need for either G-tube, J-tube or Nissen, it is recommended to get in touch with Feeding Tube Awareness organization. They have a wealth of information and products to help you. The 5p- Society can also put you in touch with families who can assist and talk with you about their experiences.
Will the size of my child’s deletion tell me how he or she will develop?
The tendency is for individuals with larger deletions to have progressively more developmental issues. Information can be found in the Journal of Medical Genetics (2001) Clinical and molecular characterisation of 80 patients with 5p deletion: genotype-phenotype correcelation. Mainardi PC, et al. You may ask for a copy of this article by emailing director@fivepminus.org.
Travel tips for those with Gtubes and feeding equipment?
Parent Veronica Feigel had these tips for you:
“Call TSA 3 days before you fly and ask them to set up a Passenger Support Specialist or PSS since you have a disabled child. The airport should send you a message giving you a name of the person who will be there to assist you and if not then someone will be there regardless, you just need to ask for them when you get to the beginning part of the security line. (Basically ask for their name or if they didn’t give a name then say your child is disabled and you are requesting a PSS for assistance) Put their medical food/formula in a ziplock bag as well as the pump because they will need to see this. The first time through in Jax they took us through the priority line and I didn’t have to take my shoes off, in Portland Maine I had to have a pat down and they swabbed my bags. Both times though they were very helpful and courteous to myself and my 2 kids. After that if I had needed a wheel chair or something then I could have asked for one. We flew southwest and at the gate I talked to the person there and they gave us pre boarding statue so we could get on before anyone else which was very helpful. I would guess other airlines would have this as well. I also shipped my formula ahead of time since I was staying with my parents, I didn’t want to take the chance it would leak on the plane. If you have any other questions please feel free to ask.”
Tips for Diapers when child has outgrown commercial brands?
Many families have posted on social media various online stores that they purchase or have purchased a variety of diapers when their child or adult has outgrown commercial brands. This list will also include swim diapers that have been found. The 5p- Society doesn’t endorse any brand listed below.
- Tranquility Slimline Original Disposable Briefs – can be found on ebay and Amazon
- UP360 – My Pool Pal has various products including swim diapers for special needs community.
- Tena Briefs
- Prevail Sleep Overs come in various sizes and can be purchased at Walmart, Amazon or medical supply stores. (example found here)
If you find more to add to this list, please send an email to director@fivepminus.org